|
People mean well, but they can say the STUPIDEST things about your breast cancer diagnosis. If you're lucky, their stupidity may tickle your funny bone and at least give you a giggle. However at a time when you are feeling vulnerable, it's not uncommon to feel intense disappointment, hurt and anger at the insensitive things people you expect more from say to you. Excuse my "Sally Sunshining" for a moment, but these insensitive comments may be a gift. Breast Cancer treatment is all about removing the malignant tumor from your body, and truth is, most of us have some malignant people in our lives as well. Consider these moronic statements as the malignant people just raising their hands saying "Me! I'm the dumb ass who does not deserve your time, your energy, your love! Kick ME to the curb!" They're making it EASY for you! (Ok, I'm totally over simplifying, and I acknowledge the intense pain that can accompany removing toxic people.) You may be better off in the long run without these people. And of course, there are those that honestly mean well but are just lacking in ability to offer appropriate support. (I affectionately refer to this group as the "ding dongs.")
Have any favorite LEAST HELPFUL things that people have said to you since diagnosis? Any strategies to deal with them? Share in comments below!
0 Comments
#Our Story is a new feature where Tribe members share reflections on their cancer diagnosis. Our first installment is by Erin Cummings. The Fallacy of Strength
“You’re so strong, you’ll beat this.” “Cancer doesn’t know who it’s messing with.” “If I know anyone who is strong enough to kick cancer’s ass, it’s you.” Even before I became a cancer patient, I was a Cancer by way of my horoscope. If you believe in these things (and I do), this gives me a seemingly impenetrable shell. To the outside world, I seem powerful, fierce, and unscathed. However, like a crab, I am completely mushy on the inside. I have often thought of this as my secret gift; underneath the tough exterior was a beautiful well of empathy for others.. When I was diagnosed with breast cancer, I was constantly told how strong I was and that I was going to beat it. It was an endless barrage of support by way of cheerleading. They had good intentions, don’t get me wrong. In fact, before I got cancer, I may have read lines from similar scripts. After all, isn’t that what we’re supposed to say: You’re so strong. You will beat this. At least, that’s what we want to be true when someone we love is diagnosed with an illness over which we don’t really have any control. However, being on the receiving end, this is what I heard: When people said, “you’ve got this,” I heard, “this should be easy for you.” When people said, “you’re so strong,” I heard, “please don’t complain.” When people said, “you’re going to kick cancer’s ass,” I heard, “I don’t really know how to be here for you right now, so I’m just going to say what I think I’m supposed to say in this situation.” The truth is that strength doesn’t mean a damn thing when you’ve been diagnosed with cancer. In some ways, I felt like the passive participant, being advised by others, by experts—like, by doctors who looked at black and white images of spots and lines and somehow knew that what they were looking at was X instead of Y and then decided which new therapy would drip from my IV bag. Or by the surgeon who meticulously sliced me open, scooped me like an avocado and zipped me back up again. Or the radiology oncologist and her team of laser wizards who radiated my body ad nauseum. When people offered to pray for my strength, I wanted to say to them, “Don’t pray for me. Pray for my doctors, that they make the right decisions for my care. Pray that my health insurance stays intact. Pray that I figure out how to do my disability paperwork because the parking at the hospital is absurdly expensive and the chemo ward doesn’t validate.” However, the biggest problem that I had with people celebrating my perceived strength was that I felt like in moments I needed to most, I wasn’t allowed to be weak. My breakdowns and my vulnerability were hidden behind closed doors. My fears and my anguish and my rage were vomited on the few people I allowed in. And they were forced to bear the brunt of it because I didn’t feel like I could share that ugly, pathetic, soft side with everyone. I wanted to say, “I’m a hack. I’m weak. I’m not strong. I’m a fucking mess and I don’t want to do this and I can’t do this and I just want to buy a one-way ticket to Mexico and lay on the beach drinking cocktails until whatever this awful disease wants to do to my body just does it already and I don’t even care if I die at this point.” And it was in those moments that I started to realize my true strength. It took me actually pushing through and making the decision every three weeks to go back and get the infusion, knowing what I would go through, but not knowing if it would be worse this time. As my estrogen levels plummeted and my hormones became as predictable as Pop Rocks, my mind went to places that I had never imagined. I went really dark. I read a story of a woman in her 90s who was diagnosed with cancer and decided against treatment and lived her life until she died. I don’t think I’ve ever been more jealous of anyone in my life. But I chose to live. I chose to live in discomfort and sometimes agony. I chose to let my body get shot up with poison. I chose to cut off beloved parts of my body. There was my strength. Maybe that’s what people had been talking about all along when they mentioned my strength, but I felt like I was discovering it for the first time. When we are diagnosed, we have a rare opportunity that most people don’t get until late in life. When it’s time for people to die, a lot of times, it just happens – a heart attack, a car accident, a tragedy, or they just get to that age where death is an inevitability. When we, as young people who are diagnosed with cancer, are asked to begin treatment, we are actually being faced with the decision of continuing or ending our own lives. Unless we are legal minors, no one will put a gun to our heads and force us to accept treatment. We could say no. We could just say, “I’m not really where I want to be in life and I think I’m just going to check out.” Yet, we press on. We move, sometimes just shuffling one foot in front of the other, in a bit of a haze, because if we stop for too long, we may not get going again. That is where we need strength. But it is important to note, that kind of strength doesn’t mean: Cancer doesn’t know what it’s up against. Or, Cancer picked the wrong girl. Even as I participated in my cancer treatment, day in and day out, there was always an element of “cross my fingers, hope this works.” Because I might be strong, and I might make strong decisions, but cancer doesn’t kill someone else who is making those same decisions because they are “weak.” At this point, many of us have known women and men and even children who were stronger than we could ever pray to be, yet died of cancer anyway. There is no shame in dying of cancer. It has nothing to do with strength. The strength lies in the ability to be treated for cancer. It takes strength to put your life and your dreams and your petty little life dramas on hold so that you can be sick for a year in hopes of getting better. I’m now learning that, in my first stages of survivorhood, I need a new kind of strength – the kind of strength that forces me to go about my day without being sucked into a vortex of fear that the cancer will come back. However, at this point, I know I’m strong enough to do that. I know that, having been faced with my own mortality and choosing to step forward, I made a choice to live life on my terms. Each and every day, I have to remind myself that I’m strong. I have to remind myself that I chose to stay here. I have to remind myself that, with that choice, comes the responsibility of making my life what I want it to be. Now, when people tell me how strong I am, I simply say, “Thank you. I am stronger today because of it.” Erin Cummings is an actress, activist, Founder of the non-profit Mittens for Detroit, and she currently sits on the Advisory Board of Cancer Free Generation, a division of Tower Cancer Research Foundation. She was diagnosed with Stage 2, HER2+ Breast Cancer two months after her wedding in 2016. She credits her superhero husband, her Breasties, and the word FUCK for getting her through her first year of marriage and cancer treatment at the same time. Our first Guest Blog by our friends at Hip Hemp! Studies show the benefits of hemp seed oil range from younger looking skin to regulating hormonal balance for menopausal support. Among its many benefits, it has been shown to lower cholesterol, help moderate blood sugar levels and boost immune systems.
The Many Benefits of Hemp Oil Hemp oil contains 25% high quality protein, polyunsaturated fatty acids, omega 6, omega 3, linoleic acid and insoluble fiber, which makes this “super oil” the perfect balance of nutrition that our bodies need. It also provides Beta-carotene, an antioxidant, which is then converted into Vitamins A, C and E. Vitamin A is an essential vitamin. Vitamin C helps synthesize collagen, which gives strength and flexibility to organs, and Vitamin E is an important antioxidant. Hemp oil also contains several minerals such as calcium, magnesium, potassium iron, zinc, and phosphorus, all which reduce risk of disease and manage chronic diseases such as diabetes, hypertension, (high blood pressure) heart disease and cancer. Other Advantages of Hemp Oil include: Improves immunity levels Reduce symptoms of PMS & menstrual cramps Reduces inflammation Improves recovery of muscles after exercise Reduces and treats dry skin and improves skin elasticity Reduces many degenerative diseases Provides nervous system support Provides detoxification Is vegetarian approved Hemp Oil Does Not Contain: GMO’s Gluten Soy Herbicides Pesticides Estrogen Peanuts References 9 Health Benefits of Hemp Oil That You Should Know. (n.d). Retrieved May 22, 2017, http://www.zliving.com/wellness/natural-remedies/9-health-benefits-of-hemp-oil-that-you-should-knowHow Healthy is Hemp? (2012) Retrieved May 26, 2017 from https://www.drweil.com/diet-nutrition/food-safety/how-healthy-is-hemp/ http://www.mynetdiary.com/foods-nutrient-needs.html#sthash.qWxKpgXT.dpuf
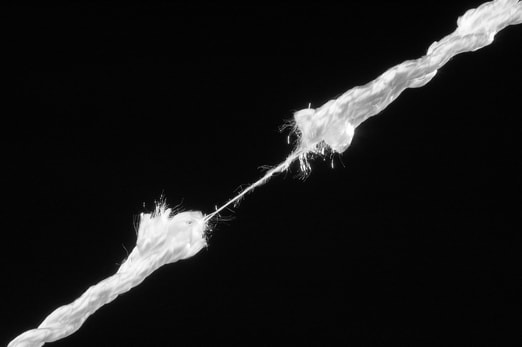
Breast cancer treatment seems to be full of unexpected “surprises,” and one high on that list is “cording” (or Axillary Webbing Syndrome, if you want to be fancy). The symptoms are best described as a really specific sensation of pulling, the kind you can pin point and trace with your finger. In fact, if you did try to trace it with your finger you may actually feel it. It’s as if there’s a guitar string running just under your skin (hence it’s common name of “cords.”). It can feel like something is tearing, or even like you’re pulling on a nerve. It does NOT feel tight in a familiar way, like say you have a tight calf muscle and then you stretch it and it feels better. It’s different. It can be severe enough to limit your movement, most often of your shoulder but can also impact elbow straightening and wrist/hand function.
Cording usually starts in your armpit and travels down into your arm, but can also start at your port (especially if it’s in your upper arm) or underneath expanders or implants. What is it? This is an excellent, and frustrating question. There is no general consensus. As a physical therapist who specializes in treating women with breast cancer, and as a Certified Lymphedema Therapist (CLT), I’ve done lots of research on this from different continuing education courses to plain old googling the interwebs. Here’s what I’ve learned: There seem to be 3 main theories of what the cord is actually made of. 1. Scar tissue that has run amok. 2. Lymphatic vessels that have hardened. 3. In the arm, the major arteries, veins and nerves run together in a bundle. Some believe the connective tissue that surrounds the bundle is what becomes fibrotic (medical word that basically means “hard.”). Anecdotally, I can tell you from working with patients, that all three make sense to me. Sometimes there is a really thick cord that starts in the armpit and seems to be scar tissue left over from lymph node dissection, or expander placement. Often times plastic surgeons tell their patients they can “clean that up” during the expander exchange surgery for implants. Other times the cording is more diffuse and webby, just like the lymphatic vessels, or can follow the exact anatomic pathway of a major artery/vein/nerve bundle. How do we get rid of it? The good news is, this is self limiting, meaning it will eventually go away on its own. A physical therapist that specializes in treating breast cancer can definitely help and make the process easier. On your own- keep using and stretching your arm as best you can, and gently massage over the cords as if you were trying to rub lotion into them. You may hear/feel a “pop” sensation, indicating one of the cords have snapped. This might feel like being on the wrong end of a zinging rubber band, but typically results in less pain with better arm motion after. Breaking the cords in this manner is not necessarily our goal- again, as we don’t know 100% what the cords are made of, and better not to just snap random things in the body- but if it happens naturally, that’s fine, no need to worry. How long until it goes away? Cording can last several months, and seems to take a few steps forward, then backward, but eventually will stop completely….until it randomly show up again for a few days and then seems to be gone for good. Typically it’s completely gone in 4 to 6 months.
Can the next generation female condom help with painful sex??
So the glories of menopause include dry, irritated vaginal skin. Typically we think only of lube, lube, lube to fix it, but the female condom could act as a barrier to protect the vagina from whatevs you want to insert into it. 😉 One end of the condom is inserted similarly to a Nuvaring, where you pinch a small, flexible circle and insert into the vagina. The other end remains outside of the body (if my description leaves more questions than answers, check out https://fc2.us.com for more information). The condom is latex free and lubricated on both sides. Anyone wanna try this and report back??? As you can imagine, many topics come up in our private #OurTribe Facebook group. Looking for a good moisturizer during radiation? Post reconstruction bra? We've got that covered. But when the topic of sex came up...well we were stumped. One member suggested pole-dancing classes, and while we still might try that, I was struck by the general lack of suggestions from these incredibly resourceful women.
I went looking for answers, and fortunately found Dr. Shannon Chavez, a Beverly Hills psychologist and Sex Therapist, whose many areas of expertise include Cancer and Intimacy. I was impressed with her Mind-Body approach, and ability to suggest very practical things (such as the best lube) to more emotional support. I felt confident she would have some answers to our questions. Luckily, Dr. Chavez was willing to offer a workshop at our Beverly Hills clinic. On October 21st, ten women bravely joined us to discuss Sex after Breast Cancer. A common component of breast cancer treatment involves placing women into menopause. The effects of menopause on their sex life was probably the number one complaint we heard. Decreased libido, vaginal dryness and pain can all result from decreased estrogen. Luckily, Dr. Chavez had some advice. We learned that the skin in the vagina can be moisturized daily just like the skin on your face! Imagine how dry, flakey skin anywhere else on your body can be itchy, irritated, and more prone to cracks and cuts. The same is true for vaginal skin. We received free samples of “moisture drops” by Hip Hemp (www.hiphemp.com/product/moisture-drops). These little drops are actually small “pearls” containing organic hemp oil, grape seed and vitamin E. It is recommended to insert vaginally at bedtime. In addition to daily moisturizing, lubrication is essential. Dr. Chavez’s favorite is from a German company, called “Pjur Med.” They offer both silicone and water based lubes. If all the moisture in the world isn’t enough to soothe your angry vagina, the newly revamped female condom might be just the thing. One end of the condom is inserted similarly to a Nuvaring, where you pinch a small, flexible circle and insert into the vagina. The other end remains outside of the body (if my description leaves more questions than answers, check out www.fc2.us.com for more information). The condom is latex free and lubricated on both sides. The material of the condom can act as a barrier between vaginal wall and penis (or whatever you choose to insert) and may reduce pain. The two hours scheduled for our workshop flew by, and with a giant basket of vibrators for us to explore, the workshop went over the allotted time. We decided we needed more- we barely touched on the emotional components surrounding your body after the invasive, life altering treatments for breast cancer. In addition, we thought the spouses would benefit from a similar workshop, and we are in the process of creating a “Couples Only” one to be held in early December. I’ll keep you posted as we learn more! For more info on sex after cancer: www.drshannonchavez.com www.sexualityresources.com (Ok so "pump" isn't the best euphemism for vagina, but "Prime the hooha" just didn't have a ring to it..)
Priming is a daily, 10 min technique to help with vaginal dryness.
You may start noticing a difference after one week, but stick with it if not. In order to work this needs to be done daily. 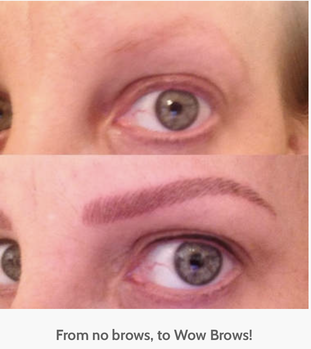 by Stacey R I am one of the very few whose brows never came back after chemo. Mind you, I went through chemo twice, which I am sure didn't help the situation. I began resenting the amount of time it took to draw on my brows in the morning and began investigating my options. There’s Latisse, which is a gel approved by the FDA to grow eyelashes, but has been used “off label” to grow eyebrows as well. Most users begin to see changes in 4 to 6 weeks, with the biggest improvement between weeks 12 and 16. Latisse doesn’t work for everyone (unfortunately, including me) and results only last as long as you use the product. Another, more extreme option was an eyebrow hair transplant. For this, they remove a strip of hair from your scalp and then graft individual hair follicles into your brow. Because you now have head hair for eyebrows, you need to trim it fairly often and may need to “train” the hair to act more, er, eyebrow-y. No thank you. After sharing my eyebrow tales of woe with a gal at my plastic surgeon’s office, she mentioned that a friend of hers did permanent makeup. No, not like the sharpie drawn on kind Michael Jackson or past-her-prime Elizabeth Taylor wore (may they rest in peace). This technique, called “microblading,” uses precise, individual strokes to recreate your brow. Because the ink in microblading is applied closer to the surface of the skin than with tattooing, it needs to be touched up every 1 to 3 years. I got them done for the first time about a year ago. It was 2 sessions, 2-3 weeks apart, and let me be clear, she basically recreated my brows from scratch. Each session lasted about 3-4 hours and the pain is minimal…truly. It's not like getting a regular tattoo, because it doesn't go as deep, so you barely feel it. It is actually kind of relaxing and she told me she's had people fall asleep in her chair. I got mine touched up last weekend and am just as in love with them as I was a year ago. They actually look better than my real brows used to look. If your eyebrows need some help, I highly recommend permanent makeup. |
AuthorJenni Rai is a physical therapist in Los Angeles, Ca who specializes in breast cancer. Archives
February 2018
Categories
All
|








 RSS Feed
RSS Feed
